This page contains helpful information about alcohol, tobacco and e-cigarettes, marijuana, prescription stimulants (e.g., Ritalin, Adderall), molly/ecstasy/MDMA, and heroin. It also provides information about alcohol and drug use among Cornellians, and harm-reduction strategies for students.
See information below about ...
Alcohol
Research shows Generation Z is drinking far less alcohol than previous generations, but it is still the most-used substance on college campuses. At Cornell, the majority of Cornellians drink moderately, or not at all (Fall 2025 Alcohol and Social Life Survey). Lots of Cornell students know how to have fun without alcohol. See our Alcohol and other Drugs Initiatives page for more data. In fact, one half of Cornell undergraduate students do not drink alcohol during their time at Cornell (Fall 2025 Alcohol and Social Life Survey). There are lots of reasons why students choose to abstain from using alcohol; these include religious beliefs, personal values, compliance with the law, health concerns, medication interactions, family history of substance misuse, or being in recovery.
Although some students are proactive about seeking therapeutic support for their drinking or drug use, many others are not aware of the harms caused by their substance misuse. Stigma and misunderstanding often prevent people from asking for help, so compassionate conversations are important. Routine screenings at medical and mental health appointments, as well as encouragement from concerned family members, friends or faculty can help people identify the issue and accept the appropriate care.
Alcohol is the third leading preventable cause of death in the United States (NIAAA, 2019), and NIAAA researches estimate that 1,825 college students die from alcohol-related unintentional injuries each year.
Every student should know …
- the rules and policies for alcohol use at Cornell
- the ABCD signs of – and what to do in – an alcohol emergency
- how Cornell’s Good Samaritan Protocol and NY State Law protect you if you call 911 for help in an AOD emergency
- how to get help if you – or a friend – is struggling with use
- how to limit negative consequences of drinking (see below)
Health risks associated with alcohol
According to the CDC (2018) and NIAAA (2018), alcohol consumption can lead to:
- increased short-term risks (e.g., accidents, injuries, alcohol poisoning, violence, unwanted sexual activity)
- a variety of longer-term physical health risks including but not limited to: high blood pressure, heart disease, stroke, liver disease, digestive problems (e.g., ulcers and gastroenteritis), and certain types of cancers (mouth, esophagus, pharynx, larynx, liver, and breast)
- exacerbated mental health problems including depression and anxiety
- social problems
- problem with academic performance, learning and memory, loss of productivity
Tips for lower-risk drinking
If you drink alcohol, try these tips to enjoy the buzz while avoiding the risks and negative consequences.
Before drinking:
- Eat! It helps your body will process alcohol more slowly (especially important for females / people assigned female at birth, who metabolize alcohol differently than males / people assigned male at birth)
- Consider ahead of time how drinking may affect your other commitments
- Bring safer sex supplies in case you or a friend hooks up
- Have a plan for getting home safely
While drinking:
- Space and pace your drinking (about one per hour)
- Sip drinks; avoid shots, funnels, chugging
- Alternate between non-alcoholic and alcoholic drinks
- Stick to beer and avoid mixed drinks
- Learn how to use the "fill" lines on a Solo cup to estimate the true number of drinks in your cup. Download a pdf (Cornell NetID required).

- Keep track of what you're drinking and how many Stick to the buzz and take a break so you don't get slide into the "Drunk Zone" (see “the biphasic response," below)
Avoid drinking:
- On an empty stomach
- If you’re feeling hungry, angry, lonely, or tired
- If you’re taking prescription medications that could affect – or be affected by – alcohol
- If you’re pregnant or think you may be pregnant
- If you’re taking prescription medications that could be affected by alcohol
Understanding BAC (blood-alcohol concentration)
Your BAC (Blood-Alcohol Concentration) is determined by milligrams of alcohol per 100 milligrams of blood, usually expressed as a percentage. For example, .10 BAC is 1 part alcohol for every 1,000 parts blood.
An “optimal buzz” is typically experienced when your BAC slowly rises to a level no higher than a .06. A DUI (Driving Under the Influence) in New York State is determined by blowing .08 or higher in a breathalyzer test.
- See the chart below to learn what happens as your BAC rises
- Try this BAC calculator to find out how different kinds of drinks affect you based on how many you drink, how quickly you drink, your weight, and your biological sex.
- Learn about why your sex gender matters when it comes to drinking alcohol.
- See our Alcohol Rules & Policies page to learn about how your BAC effects your ability to drive legally.

The biphasic (two-phase) response to alcohol
When a person consumes a moderate amount of alcohol slowly, the alcohol produces a mild “up” feeling – or a “buzz.” This is what most people are looking for and enjoy when they’re drinking.
However, there is a point of diminishing returns when drinking alcohol. The buzz will not get better with more alcohol. In fact, drinking more alcohol at this point can lead to more negative feelings – like fatigue, moodiness, or dysphoria. For most people, the point of diminishing returns happens when their BAC is about .06.
This “up” feeling, followed by a “down” feeling if you drink too much, has been described as the biphasic response to alcohol:
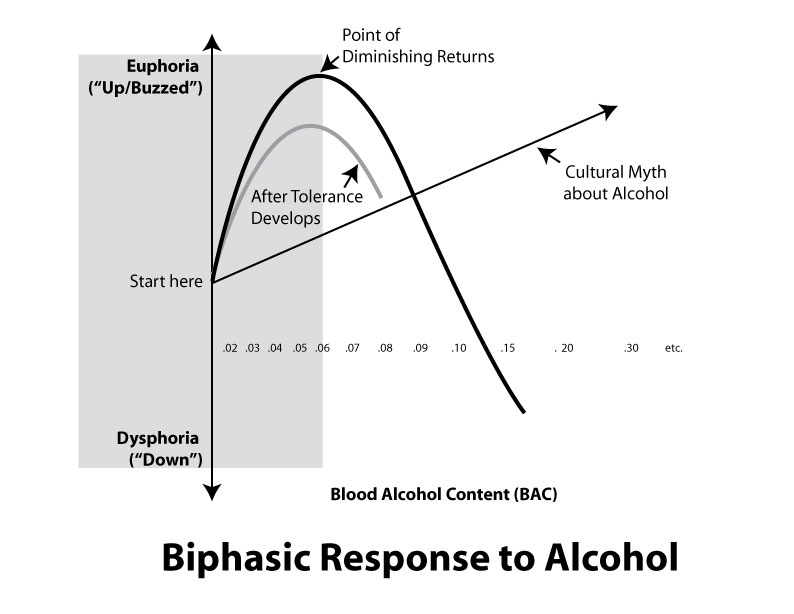
See the tips above (“Enjoy the buzz ... reduce the risks” and “Understanding BAC”) to learn strategies for enjoying alcohol without passing the point of diminishing returns.
Think you may have a problem?
Please see our Alcohol & Other Drug Services page for information about the individual counseling and support groups we offer, our BASICS program, and the many campus and community resources available to you.
Tobacco & e-cigarettes
The vast majority of students at Cornell do not smoke, and tobacco use among college students has decreased significantly over the last 15+ years – especially the use of cigarettes and chewing tobacco. That said, use of e-cigarettes is on the rise.
What to know …
- the risks of smoking and chewing tobacco
- the risks of e-cigarettes
- the gist of Cornell’s smoking policy
Learn more about ...
Tobacco / Cigarettes
If you smoke or chew ...
Tobacco is a plant, the leaves of which are smoked, chewed, or sniffed to achieve a variety of effects. Tobacco contains the chemical nicotine, which is an addictive substance. Tobacco smoke contains more than 7000 chemicals, 69 of which are known to cause cancer. Tobacco that is not burned is called smokeless tobacco. Including nicotine, there are 29 chemicals in smokeless tobacco that are known to cause cancer.
- Overwhelming scientific evidence assembled by the U.S. Surgeon General, Centers for Disease Control, Environmental Protection Agency, and World Health Organization, demonstrates that tobacco is a profound agent of deadly diseases, responsible for millions of deaths worldwide each year both to tobacco users and non-users.
- Evidence suggests that short-term exposure to secondhand smoke, even outdoors, puts people at increased risk, especially those with pre-existing cardiac and pulmonary illness.
- Adolescent brains, because of their level of development, are uniquely vulnerable to the effects of nicotine and nicotine addiction. Exposing the undeveloped adolescent brain to nicotine increases the chance that the brain will become essentially hardwired for nicotine. That is largely why about 90% of adult smokers started before age 18.
- Those who wait until the brain is fully developed (about age 25) are unlikely to become lifetime users. The longer use is delayed, the lower is the likelihood of lifetime addiction.
E-cigarettes / Vapes / Juuls
If you vape or Juul ...
E-cigarettes are a type of electronic nicotine delivery systems (ENDS). More commonly called “e-cigs,” “e-hookahs,” “JUULS,” and “vapes,” e-cigarettes are the most commonly used nicotine product among youth. These battery-powered devices heat a liquid into an aerosol that the user inhales. The liquid usually contains nicotine, flavoring, and other additives. E-cigs are largely marketed to kids; they come in fun shapes, sizes, flavors, and colors. But they aren’t harmless.
- The risks of e-cigarettes include an outbreak of lung injury associated with vaping.
- Nicotine exposure in those younger than 25 disrupts the growth of brain circuits that control attention, learning, and susceptibility to addiction.
- E-cigarettes contain high levels of nicotine. Studies have shown that teenagers who Juul have been expose to nicotine in levels that could significantly increase the potential for early nicotine addiction.
- High-wattage vaporizers may also generate significant amounts of formaldehyde and other known toxins. E-cigarette users have been found to have higher levels of these chemicals.
- E-cigarette fumes are heated by a metal coil. Users of e-cigs can be exposed to toxic metals, and to metals that are toxic when inhaled, such as magnesium and zinc.
- Juuls have been found to emit higher levels of benzoic acid than other e-cigarettes. Benzene has been named as the largest single known cancer-risk air toxin in the United States.
- Flavored e-cigs often contain a chemical compound called diacetyl. This compound is associated with a rare lung disease called bronchiolitis obliterans, which causes permanent damage to the bronchioles in the lungs.
The effects of nicotine exposure can be long-lasting and include lower impulse control and mood disorders. If you already use tobacco or e-cigarettes and want to quit, make an appointment with a Behavioral Health Consultant at Cornell Health. Cornell Health’s pharmacy also sells nicotine replacement products (gum and patches).
If you want help cutting back or quitting …
Please see our Tobacco & Nicotine Cessation Services page for information about support for quitting, including behavioral health consultations, free Quit Kits, and nicotine replacement therapies (NRTs). And don't give up! Tobacco dependence is a chronic health condition that often requires repeated intervention and multiple attempts to quit.
Other drugs
The vast majority of Cornell students do not use other drugs. Of the other drugs used by students, cannabis is the most common. In surveys of Cornell students, five percent or fewer report using drugs other than cannabis, alcohol, or tobacco (Fall 2025 Alcohol and Social Life Survey).
Learn more about …
Cannabis / Marijuana
The effects of cannabis can vary widely, depending on the potency of the drug, any tolerance you may have built up, the location of where it is used (e.g., how safe you feel in that environment), and other factors about how you’re feeling at the time of use.
Short-term risks: While you won't overdose on cannabis, short-term risks include impairment to judgment and complex coordination (e.g., driving is NOT recommended), increased heart rate, and other symptoms such as paranoia, mild hallucinations, or anxiety. For people sensitive to the chemical agents sprayed on cannabis plants, use may cause painful migraine headaches. Cannabis can also impair memory and other cognitive functions for up to 48 hours after using.
Long-term risks: There is little evidence to suggest that cannabis causes long-term harm to memory and cognitive functions (effects usually fade about 48 hours after use). However, with continued use, you CAN become dependent on – and addicted to – cannabis. Chronic, heavy use can also damage your lungs and contribute to both depressive episodes and increase chance of suicidal thoughts. As with any drug, chronic exposure as a child or adolescent could result in changes in your brain since it is developing rapidly during these years.
About "Edibles": The term "edible" can refer to cannabis products purchased at a store (e.g., "gummies," chips, hard candies), or homemade items people create themselves, usually infusing cannabis into butter to be baked into brownies, cookies, etc. In homemade edibles, it's hard to measure the dose of THC in any particular part of the batch, so there can be significant variance (i.e., one person might not get any effects, while someone else might get a lot more than they bargained for).
In either case, when compared to smoking cannabis, edibles take longer for the effect to kick in. Once it does, however, it's usually more intense and lasts longer than the effects of smoked cannabis. This can sometimes lead to people taking additional doses early on if they aren't feeling any effects, and then being way in over their heads. It is not uncommon for people to go to the ER after using edibles because the high was overwhelming / debilitating. Read more: "7 Things You Need to Know About Edibles."
Cross-fading: a word of caution...
Using different substances at the same time can be especially risky. For example, if combining alcohol and cannabis (sometimes referred to as "cross-fading"), each substance amplifies the effect of the other, so the resulting intoxication / high is significantly more than the sum of its parts. The combination of alcohol and cannabis can lead to a number of anxiety problems, including paranoia and panic attacks.
NY State Law and campus policy: While NY State legalized the recreational use of cannabis for adults over the age of 21, cannabis use remains prohibited on campus. Cornell University is subject to federal laws that expressly prohibit the possession, use or distribution of cannabis on university property or as part of university-sponsored events.
Learn about how to take a cannabis tolerance break (used with permission from University of Vermont).
Prescription stimulants (e.g., Ritalin, Adderall)
Ritalin, Adderall, and other prescription stimulants are “central nervous stimulants” commonly prescribed to help people diagnosed with Attention Deficit / Hyperactivity Disorder (ADHD) focus and concentrate. Nationally, some people without prescriptions take these stimulants in hopes of increasing mental alertness and decreasing fatigue – while studying, or in social settings. (Note that it is illegal to take prescription stimulants without a doctor's prescription.)
Short-term risks: Depending on the dosage, you may find yourself feeling depressed and irritable after the peak effect of the drug has passed. Other side effects include dehydration, hot flashes, nervousness, appetite suppression, stomach pains, palpitations, nausea, heavy sweating, decreased libido, and headaches. Prescription stimulants interact negatively with a number of other substances; if you’re experiencing problems after taking a prescription stimulant, seek medical help (you can call us 24/7 at 607-255-5155).
Long-term risks: If misused or abused, prescription stimulants can be addictive, and cause serious withdrawal symptoms when stopped. Potential overdose is also a concern. Other health risks include insomnia, digestive problems, vomiting, irregular heartbeat (cardiac arrhythmia), extremely high blood pressure, allergic reaction, loss of appetite, sexual dysfunction, abnormal behavior, confusion, nervousness, psychotic episodes, and seizures.
Molly / Ecstasy / MDMA
The MDMA in Molly and ecstasy usually produces a mild, euphoric state within 20-40 minutes after ingesting a tablet, with the peak effect occurring 60-90 minutes after. Its stimulant effects can increase your energy and decrease appetite.
Short-term risks: Potential short-term negative effects may include anxiety, confusion, depression, sleep problems, and paranoia. Also, people may experience muscle tension, involuntary teeth clenching, increased heart rate, increased blood pressure, and increased body temperature. Deaths have been associated with this substance, usually as a result of heat stroke. If you decide to use ecstasy, it is important to stay cool and well-hydrated. Ecstasy can also be especially dangerous for people with heart problems.
Long-term risks: Evidence suggests that long-term use or a single high dose can cause a long-term loss of serotonin, an important chemical in the brain that regulates mood. This sort of damage could cause subtle but significant impairment to cognitive abilities, memory, arithmetic calculation, complex attention, and increased impulsiveness. If you have used Molly / ecstasy / MDMA and are worried about any effects you’re experiencing, please schedule an appointment with a counselor or medical provider at Cornell Health.
Learn about supplements to reduce the risks and side effects of MDMA.
Heroin
Heroin is snorted, smoked, or injected. It can elicit a warm, euphoric feeling – although responses vary depending on dosage, the purity, and your own physical condition. Less than 1 percent of Cornell students report having used heroin, although its use is growing in many parts of the country, including Tompkins County.
Short-term risks: The most serious short-term risk associated with heroin is overdose / sudden death (most common when injected). Other less serious effects can include experiencing nausea, constipation, diminished sex drive, and withdrawal.
Long-term risks: Heroin is highly addictive. Additionally, injecting heroin is linked with infections (like hepatitis, HIV, or blood poisoning) and abscesses. The Harm Reduction Coalition offers reliable, unbiased information about heroin.
If you inject heroin: It's important to use a sharp, sterile syringe, clean works, and fresh sterile water. If possible, use a fresh needle every time. Avoid sharing needles with others. If you don't have new needles, go to an exchange: Ithaca hosts the only rural syringe exchange in New York. If you have your own needles, be sure to dispose of them safely (see information about Disposing of medications & sharps on our Pharmacy page).
If you want help cutting back or quitting …
Please see our Alcohol & Other Drug Services page for information about the individual counseling and support groups we offer, and the many campus and community resources available to you.

